Craniocervical pathologies
Craniocervical pathologies are complex conditions affecting the junction between the skull and upper cervical spine, commonly referred to as the craniocervical junction. This highly specialised area contains critical neurological structures including the brainstem, upper spinal cord, vertebral arteries, and surrounding stabilising ligaments and bones.
Disorders affecting the craniocervical junction may cause instability, neurological compression, cerebrospinal fluid flow abnormalities, pain, and progressive neurological symptoms. These conditions can significantly affect mobility, balance, coordination, swallowing, and overall neurological function.
Craniocervical pathologies may include Chiari malformation, basilar invagination, atlantoaxial instability, craniovertebral junction abnormalities, congenital deformities, trauma-related instability, inflammatory conditions, and degenerative disorders.
At Spine Focus UK, Mr. Taofiq Desmond Sanusi provides specialist assessment and advanced treatment for complex craniocervical disorders using modern imaging, evidence-based neurosurgical techniques, and highly individualised treatment planning.
Early diagnosis and specialist management are essential to protect neurological function, improve symptoms, restore stability, and prevent progression of neurological complications.
Understanding Craniocervical Pathologies
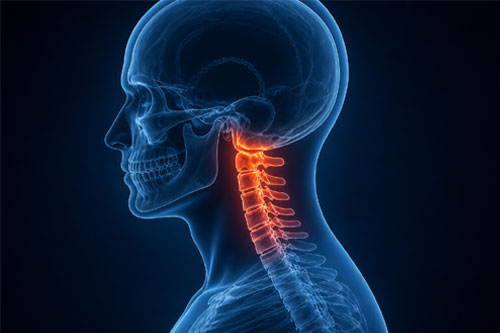
The craniocervical junction is the highly specialised region where the skull meets the upper cervical spine. This area plays a critical role in supporting the head, protecting the brainstem and upper spinal cord, and allowing controlled movement of the head and neck.
Because of the complexity of this region, disorders affecting the craniocervical junction can have significant neurological consequences. Compression of the brainstem, spinal cord, or surrounding structures may lead to pain, weakness, balance difficulties, swallowing problems, dizziness, and progressive neurological symptoms.
Craniocervical pathologies are often highly complex and require specialist neurosurgical assessment, advanced imaging, and detailed treatment planning.
At Spine Focus UK, specialist evaluation focuses on understanding the structural abnormalities, neurological involvement, spinal stability, and cerebrospinal fluid dynamics affecting each patient in order to develop an individualised treatment strategy.
What Conditions Affect the Craniocervical Junction?
Chiari I Malformation
Chiari I malformation occurs when the lower part of the brain extends downward through the opening at the base of the skull, potentially affecting cerebrospinal fluid flow and compressing neurological structures.
Patients may experience:
- Headaches
- Neck pain
- Balance problems
- Dizziness
- Numbness or weakness
- Swallowing difficulties
- Syringomyelia
Basilar Invagination
Basilar invagination occurs when the upper cervical spine migrates upward toward the base of the skull, potentially compressing the brainstem and spinal cord.
This condition may be congenital or develop due to inflammatory or degenerative disease.
Atlantoaxial Instability
Atlantoaxial instability involves excessive movement between the first and second cervical vertebrae.
Instability may result from:
- Trauma
- Congenital abnormalities
- Inflammatory conditions
- Connective tissue disorders
- Degenerative changes
Severe instability may place the spinal cord and brainstem at risk.
Craniovertebral Junction Abnormalities
Various congenital or acquired abnormalities may affect the alignment and stability of the craniovertebral junction.
These conditions may disrupt neurological function or cerebrospinal fluid flow.
Trauma and Fractures
Traumatic injuries involving the upper cervical spine and skull base may cause instability, fractures, spinal cord compression, or vascular injury.
These injuries often require urgent specialist neurosurgical assessment.
Common Symptoms of Craniocervical Pathologies
Symptoms vary depending on the specific condition and the degree of neurological involvement.
Common symptoms include:
- Neck pain
- Occipital headaches
- Dizziness
- Balance problems
- Numbness or tingling
- Weakness
- Difficulty swallowing
- Visual disturbances
- Hearing changes
- Coordination problems
- Reduced mobility
- Gait disturbance
- Neurological deterioration
Some patients may also develop symptoms related to spinal cord compression or cerebrospinal fluid flow abnormalities.
Diagnosis of Craniocervical Disorders
Accurate diagnosis requires comprehensive neurological evaluation and advanced imaging studies.
Investigations may include:
- MRI scans
- CT imaging
- Dynamic cervical spine imaging
- Cine MRI cerebrospinal fluid flow studies
- Neurological examination
- Assessment of spinal stability
- Vascular imaging in selected cases
Advanced imaging allows detailed assessment of the brainstem, spinal cord, alignment, instability, and cerebrospinal fluid flow at the craniocervical junction.
Non-Surgical Management
Some patients with mild or stable symptoms may initially benefit from conservative treatment.
Non-surgical treatment options may include:
- Physiotherapy
- Pain management
- Activity modification
- Neurological monitoring
- Regular imaging follow-up
- Medication for symptom control
Conservative management is carefully tailored to the specific condition and severity of symptoms.
Surgical Treatment for Craniocervical Pathologies
Surgery may be recommended when patients develop neurological symptoms, spinal instability, progressive compression, cerebrospinal fluid obstruction, or worsening quality of life.
Surgical goals may include:
- Relieving brainstem or spinal cord compression
- Restoring stability
- Correcting alignment abnormalities
- Improving cerebrospinal fluid flow
- Preventing neurological deterioration
Decompression Surgery
Decompression procedures may be performed to relieve pressure on the brainstem, spinal cord, or surrounding neurological structures.
Stabilisation and Fusion
Craniocervical instability may require stabilisation using specialised instrumentation and spinal fusion techniques.
Advanced Microsurgical Techniques
Modern microsurgical and image-guided techniques allow highly precise treatment of complex craniovertebral conditions while minimising risk to surrounding neurological structures.
The Importance of Specialist Neurosurgical Assessment
Craniocervical pathologies are highly specialised conditions requiring expert evaluation by experienced neurosurgical specialists.
Careful assessment is essential to determine:
- The underlying structural abnormality
- The degree of neurological involvement
- Spinal stability
- The presence of cerebrospinal fluid obstruction
- The safest treatment approach
Early diagnosis and specialist management may help prevent progression of neurological symptoms and long-term complications.
Advanced Craniocervical Care at Spine Focus UK
Spine Focus UK provides specialist diagnosis and treatment for complex craniocervical disorders and advanced neurosurgical conditions.
Mr. Taofiq Desmond Sanusi is a Consultant Neurosurgeon and Complex Spine Surgeon with advanced fellowship training in complex spinal and craniovertebral pathology, minimally invasive spinal surgery, and cerebrospinal fluid disorders.
Patients receive comprehensive, evidence-based care using advanced imaging, modern neurosurgical techniques, and personalised treatment planning focused on long-term neurological protection and quality of life.
Frequently Asked Questions
Common questions about Craniocervical pathologies, symptoms, diagnosis, treatment options, and recovery.
What are craniocervical pathologies?
Craniocervical pathologies are conditions affecting the junction between the skull and upper cervical spine, involving neurological structures, spinal stability, and cerebrospinal fluid flow.
What symptoms can craniocervical disorders cause?
Symptoms may include neck pain, headaches, dizziness, balance problems, weakness, numbness, swallowing difficulties, and neurological symptoms.
What is the craniocervical junction?
The craniocervical junction is the region where the skull meets the upper cervical spine and contains critical neurological and vascular structures.
What conditions affect the craniocervical junction?
Conditions may include Chiari malformation, basilar invagination, atlantoaxial instability, craniovertebral abnormalities, trauma, and degenerative disorders.
How are craniocervical pathologies diagnosed?
Diagnosis usually involves MRI scans, CT imaging, neurological examination, spinal stability assessment, and cerebrospinal fluid flow studies.
Can craniocervical disorders be treated without surgery?
Some patients with mild or stable symptoms may benefit from conservative management including physiotherapy, pain management, and monitoring.
When is surgery recommended for craniocervical disorders?
Surgery may be recommended when patients develop neurological compression, spinal instability, cerebrospinal fluid obstruction, or progressive symptoms.
What surgical treatments are available?
Surgical treatment may involve decompression, stabilisation, spinal fusion, or correction of craniovertebral abnormalities depending on the condition.
Can craniocervical instability become serious?
Yes. Severe instability may place the brainstem and spinal cord at risk and may lead to progressive neurological deterioration if untreated.
Why is specialist neurosurgical assessment important?
Craniocervical disorders are highly specialised conditions requiring advanced imaging, neurological assessment, and expert treatment planning to achieve safe and effective outcomes.
Need Specialist Advice?
Spine Focus UK provides specialist assessment and advanced treatment for complex spinal and neurosurgical conditions.
Book a Consultation